The Residential Program Management Institute (RPMI) adopts a policy-driven, experiential, and performance-based learning model designed specifically for adult professionals working in residential human services. This model integrates andragogy, real-time application, and data-driven monitoring to ensure competency—not just knowledge.
Andragogy Approach
(Adult Learning Model)
Experience-Based Learning: Participants bring real workplace scenarios into the training environment.
Problem-Centered Approach: Learning focuses on solving real residential program challenges (e.g., incident response, medication errors).
Immediate Application: Every concept taught is directly tied to on-the-job performance.
Self-Directed Learning: Participants engage in reflection, decision-making, and peer learning.
Real-Time In-Program Training
Example:
- Reviewing policy
- Simulating medication pass
- Completing MAR documentation
- Supervisor evaluation using compliance indicators
Staff are not just trained—they are validated in real performance conditions.
RHSDM (Residential Human Services Data Management)
Data Collection: Daily progress notes, MAR logs, incident reports
Monitoring Indicators: Each policy includes a measurable compliance metric
Performance Dashboards: Track staff competency and program outcomes
Quality Assurance Integration: Training feeds directly into audits and evaluations
Policy: Medication Documentation
Indicator: % of error-free MAR entries per staff
Action: Staff retrained if performance falls below threshold
Training is not theoretical—it is continuously measured, validated, and improved.
Practical vs Theoretical Learning (Balanced Model)
Learning
policies, regulations, and risks
Learning
situations
Fire Safety & Evacuation
- Theory: Fire risks and protocols
- Practice: Live evacuation drill with timing and evaluation
Behavioral Support
- Theory: De-escalation principles
- Practice: Role-play crisis intervention scenarios
Policy-Based Experiential Training Structure
Policy Purpose
- Why the policy exists
- Risks it prevents (legal, safety, ethical)
Staff Responsibilities
- Clear, role-based duties
Real-Time Scenario
- Example: resident refusal, medication error, behavioral escalation
Hands-On Exercise
- Documentation (MAR, progress notes)
- Procedure execution (medication pass, evacuation drill)
Monitoring Indicator
- Measurable compliance metric
- Example: incident report submission time, documentation accuracy rate
Integration with RPMI Core Modules
Client Rights Protection – Role-play advocacy scenarios + compliance audits
Confidentiality (HIPAA) – Data handling simulations + breach response drills
ISP Implementation – Daily support alignment exercises
Incident Reporting – Real-time report writing and supervisor review
Infection Control – Hygiene audits and environment inspections
Quality Assurance – Mock audits and corrective action planning
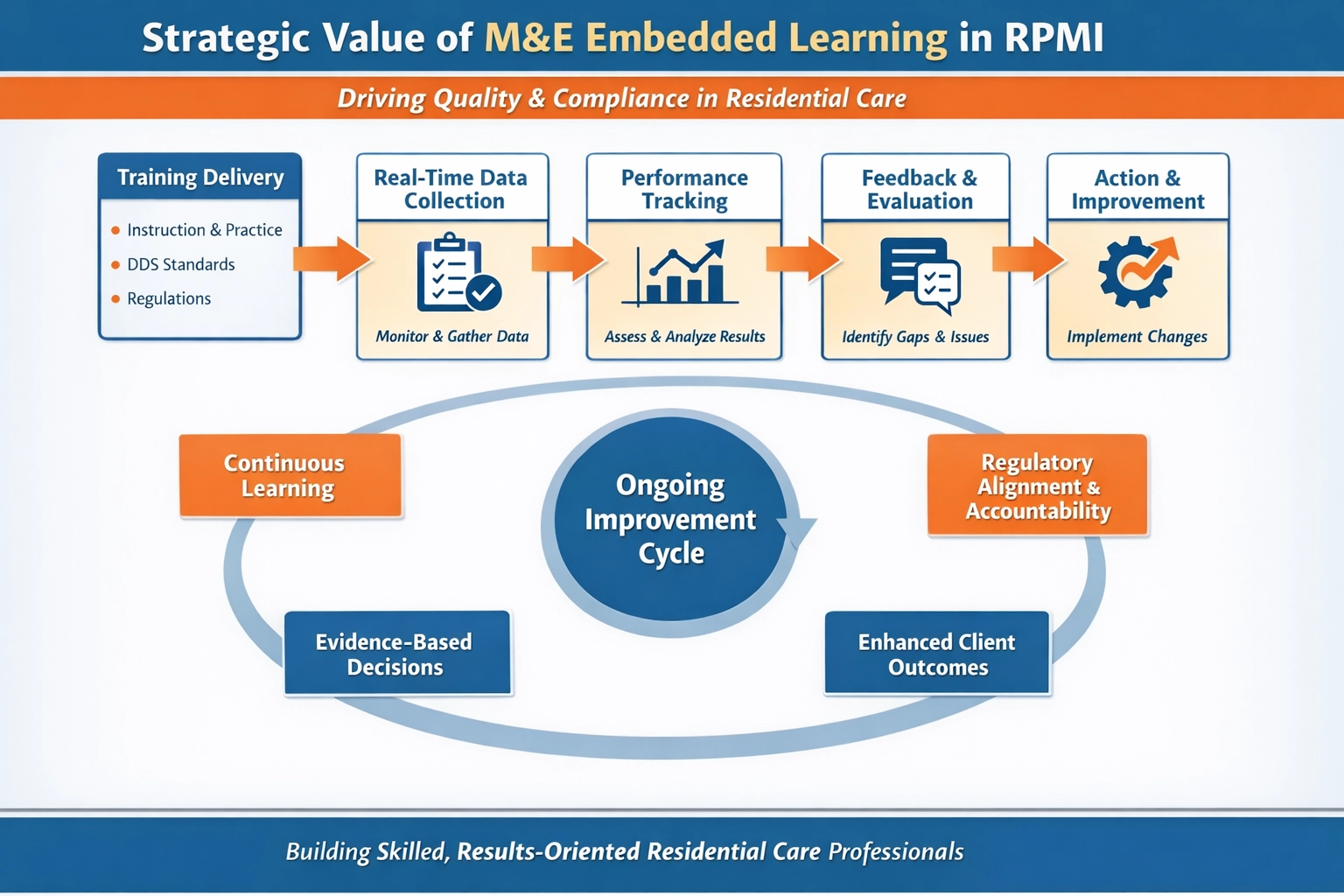
Monitoring & Evaluation (M&E) Embedded Learning
The Core Problem RPMI Solves
Residential programs rely on:
- Progress notes
- Medication Administration Records (MAR)
- Incident reports
- Behavioral tracking logs
- ISP documentation
However, most staff:
- Use tools without understanding how they were designed
- Collect data without linking it to indicators
- Document events without measuring outcomes
Why M&E Must Be Embedded (Not Separate)
RPMI does not treat M&E as a separate subject. Instead, it is embedded into every policy, module, and training activity.
- Administering medication → generates compliance data
- Writing progress notes → generates outcome data
- Responding to incidents → generates risk indicators
Bridging the Clinician–Data Gap
Clinicians and residential staff are service experts—but not trained data analysts.
- Baseline data
- Indicator types
- Data tools design
Weak linkage between documentation and program performance
Teaching the Origin of Indicators
RPMI introduces a foundational concept:
Indicators are not random—they are derived from program design and policy requirements.
Understanding Indicator Types (RPMI Framework)
Input → Output → Outcome Measurement
Data Literacy for Residential Professionals
RPMI equips staff with practical data intelligence, not advanced analytics.
Datasets: Collections of structured program data (e.g., incident logs)
Data Elements: Individual fields (date, time, resident ID, event type)
- Definition
- Numerator / Denominator
- Data source
- Frequency
- Target
- Numerator: Reports submitted within 24 hours
- Denominator: Total incidents
- Target: 95% compliance
Tool Design Awareness
Why Each Certification Level Must Learn M&E
RPMI aligns M&E competencies with career progression:
CRPM-RSS (Residential Support Staff)
CRPM-PM (Program Manager)
Responsible for program performance and compliance
CRPM-RD (Residential Director)
Oversees multiple programs and quality assurance
CRPM-EL (Executive Leadership)
Responsible for strategy, funding, and organizational outcomes
Final Positioning Statement
RPMI embeds M&E into training because data is the language of quality, safety, and accountability in residential care.
Every action becomes measurable, improvable, and accountable
RPMI uniquely integrates M&E methodology into training delivery:
Input: Training sessions, materials, simulations
Process: Participation, engagement, exercise completion• Process: Participation, engagement, exercise completion
Output: Skills demonstrated (documentation, response accuracy)
Outcome: Improved staff performance and resident safety
Impact: Higher program quality and regulatory compliance
Certification-Linked Competency Model
Training directly feeds into CRPM certification outcomes:
- Operational competence
- Policy compliance
- Decision-making in real scenarios
RPMI Learning Philosophy (Summary)
Residential Program Policy-Based Practice Training Manual. Experiential Training for Residential Staff
- Client Rights Protection
- Confidentiality & Privacy (HIPAA)
- Individual Service Plan (ISP) Implementation
- Medication Administration
- Medication Documentation
- Incident Reporting
- Abuse and Neglect Reporting
- Emergency Response Procedures
- Fire Safety and Evacuation
- Behavioral Support and Crisis Intervention
- Infection Control and Hygiene
- Daily Progress Notes Documentation
- Staff Communication and Shift Handover
- Resident Supervision and Safety Monitoring
- Transportation and Community Safety
- Food Safety and Nutrition Support
- Program Data Collection and Monitoring
- Quality Assurance and Program Audits
- Professional Conduct and Ethics
- Staff Self-Care and Burnout Prevention